|
4īowen's disease, VIN III, and carcinoma in situ are clinically synonymous terms. The incidence of progression to a malignant invasive process is relatively low (10% to 15%), and the time frame for progression may span several years. VIN lesions are sufficiently atypical to be considered premalignant. VIN is histologically divided into three categories: VIN I (mild dysplasia), VIN II (moderate dysplasia), and VIN III (severe dysplasia and carcinoma in situ). Vulvar intraepithelial neoplasia is a hyperplastic squamous lesion with atypia that is confined to the epithelium. Management is best accomplished by wide excision and careful postoperative evaluation. Characteristically, it is localized to the vulva. 1 Verrucous carcinoma may involve large areas of the vulva, and it has a pushing rather than an infiltrative border. The lesion, first described by Buschke and Lowenstein as a giant condyloma, 2 is associated with the HPV 6 viral subtype. 
Verrucous carcinoma of the vulva appears as a large condyloma or a lesion suspicious for invasive carcinoma. Recurrent viral cutaneous expressions usually are managed with alternative treatments or combinations of treatments. Intralesional or systemic administration of interferon is another therapeutic option that usually is reserved for recalcitrant lesions. 
Cryotherapy, laser vaporization, and electroexcision or desiccation are other methods of treatment. Control of epithelial viral expression can be accomplished with topical agents such as trichloroacetic acid, bichloracetic acid, podophyllin or its derivatives, or topical 5-fluorouracil (5-FU). Eradication of the virus from the epithelium is not clinically possible. Treatment consists of destruction of the cutaneous manifestations of the HPV infection. Condylomata showing acanthosis, parakeratosis and koilocytotic changes. Immunosuppressed states and pregnancy are associated with enlargement and progression of condylomatous lesions (Fig. Some HPV infections may progress to vulvar intraepithelial neoplasia (VIN) and an even smaller segment may progress further to frankly invasive squamous cell carcinoma of the vulva, but the majority of lesions are limited to the HPV cutaneus expression known as the venereal wart or condyloma. Even if only clinically expressed HPV is considered, it is now one of the most common sexually transmitted diseases. 1 There is no reliable method of identifying subclinical or dormant infection. Although it is difficult to estimate the incidence or prevalence of the infection, estimated percentages of patients with clinical and subclinical HPV infection in some college populations exceed 40%. 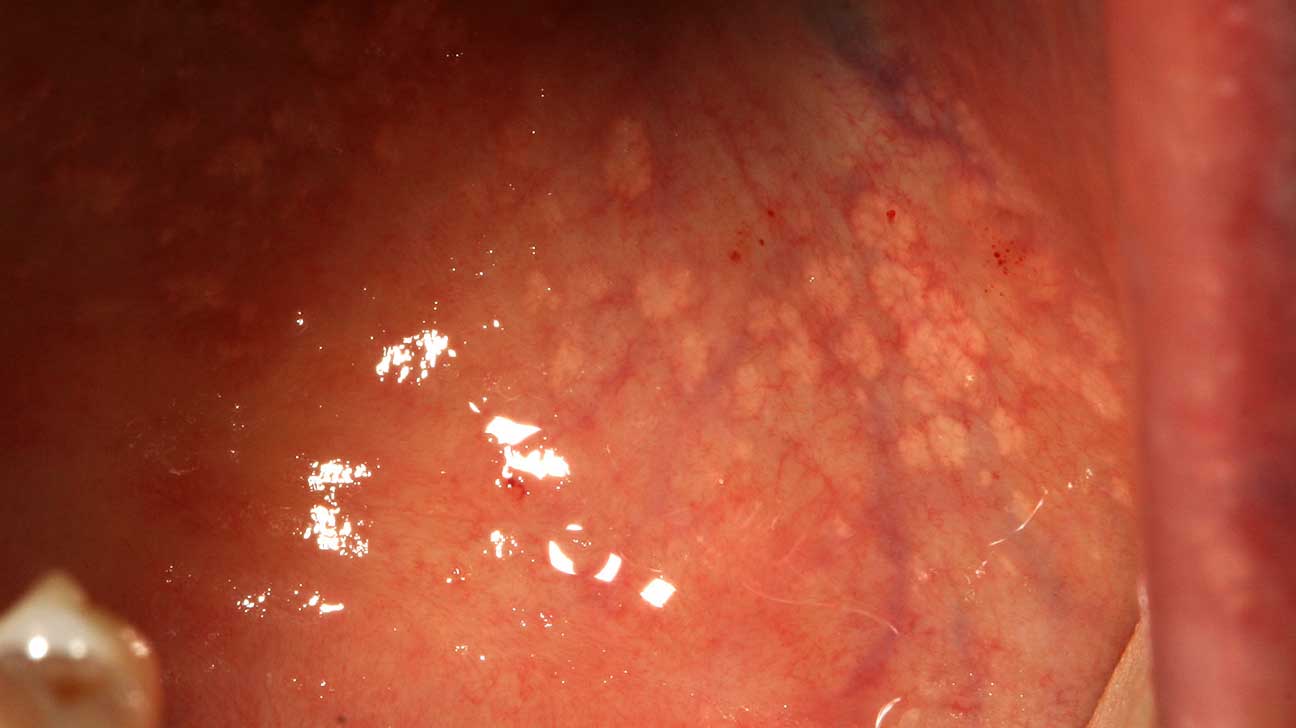
3 This increase is partly attributable to advancements in diagnostic techniques, such as polymerase chain reaction and DNA hybridization techniques. 1 The incidence of the diagnosis of vulvar, vaginal, and cervical HPV lesions has increased significantly in the last three decades. 
2 HPV subtypes that are associated with a higher incidence of malignant transformation on the cervix, specifically HPV 16, 18, 31, and 35, may be present in vulvar lesions. HPV 2, the virus associated with common epithelial warts, also is seen in the squamous epithelium of the vulva. 1 The HPV subtypes that are most frequently encountered on the vulva are HPV 6 and HPV 11. Multiple vulvar condylomata acuminata.Īlthough there are more than 60 subtypes of HPV, relatively few affect the vulva.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
